Treatment of Hyperfunction in Children
Overview:
There are numerous techniques and methods that a speech and language pathologist can
employ to treat hyperfunctional voice disorders in children. These methods aim
to decrease detrimental vocal behaviors, change the format of voice production,
and enable the healing of vocal fold tissue due to injury. Research has proven
voice therapy to be effective, either alone or in conjunction to other treatment
methods such as surgery or medications (Branski, 2011).
Intervention for vocal hyperfunction in children consists of education, which includes
awareness of voice behaviors and altering improper vocal behaviors, vocal
hygiene programs, direct vocal therapy, and generalization activities. Surgery
is an option, yet is often not preferred ("Hyperfunction Kids," n.d.).
Factors to consider:
An SLP must weigh various factors before procuring a treatment plan. The individual
child and his/her disorder must be assessed holistically. Therapy decisions
depend largely on the age of the child. Boone (2005) states that vocal
hyperfunction, a functional disorder likely caused by vocal polyps or nodules,
is the most common voice disorder found in children. He cautions the therapist
to clarify the cause of the voice disorder prior to planning intervention, as if
an organic or neurological etiology is present, a different treatment plan may
be necessary.
There are other factors to consider to assist an SLP determine an
appropriate intervention plan. These include: “vocal fold tissue health, vocal demands
of the patient, baseline phonatory behaviors, and patient compliance.” The
therapist must bear in mind that different clients with identical disorders may
require different therapies (Branski, 2011).
Goals of therapy:
All hyperfunctional voice disorders are characterized by increased laryngeal and/or
supralaryngeal muscle tension. The primary goal of treatment is to decrease this
tension during voice production, thereby improving one’s voice (Branski, 2011). Additionally,
the goal of therapy is to ingrain in the child a “healthy, non-abusive voice
production pattern (Latrobe, n.d.)." By reducing laryngeal hyperfunction and increasing
laryngeal health, the possibilities of edema, vocal nodules, polyps, and contact
ulcers will be decreased, thereby improving one’s voice and removing the
necessity of surgery("Hyperfunction Kids," n.d.).
Facilitating Techniques:
There are many facilitating techniques that can be employed to help improve the voice
of children with vocal hyperfunction. Boone et al. (2005) suggests the following
techniques: changing horizontal/vertical focus, changing loudness, chewing,
establishing a new pitch, eliminating hard glottal attack, opening mouth,
counseling, masking, pushing, and the yawn-sigh technique.
Prior to implementing facilitative techniques, it is crucial for the SLP to assist the
child in identifying the misuse and abuse of his/her speech mechanism. A
baseline of misuse should be established. If the child is aware of the instances
in which s/he misuses his/her voice, s/he may automatically decrease such
instances. Tally marks or other graphs can be used, to visually show the child
of his/her progress ("Hyperfunction Kids," n.d.). Additionally, the SLP would counsel the child and help
him/her identify the problem and its implications.
Changing horizontal/vertical focus: Sometimes a child produces
sounds by holding the tongue too far back or high in the oral cavity, yielding a
deep voice, or holding the tongue too high or to the front, yielding a thin,
babyish voice. The SLP could utilize imagery to help the client change the focus
of where the voice is being made.
Changing loudness: This method is employed if one’s voice is
excessively loud or soft. A hearing test should be administered to rule out
other possibilities for an overly loud voice. Dr. Boone suggests a five step
process to lessen the loudness including a whisper, quiet voice, normal voice,
talking across the room voice, and yelling. To increase one’s loudness,
techniques such as discussing the reason of the quiet voice, letting the child
listen to a recording of his/her voice, establishing an appropriate pitch level,
and respiration training, can be employed.
Chewing: The purpose of this technique is to teach the child to
open his/her mouth while speaking, to decrease the tension or strain. The child
should look in a mirror while opening and closing mouth in an exaggerated
chewing motion. Then the child slowly says one-syllable words, and then longer
words, and then phrases, while still chewing. The chewing is decreased after a
duration of therapy.
Establishing a new pitch: The purpose of establishing a new pitch
is to “improve vocal quality and loudness (Boone et al., 2005).” The SLP plays a
recording of the child’s voice, then imitates a pitch, as well as uses a pitch
analyzer (i.e. Visi-Pitch.) Once an appropriate pitch is found, the child can
begin to practice speaking with it.
Eliminating Hard Glottal Attack: The purpose of eliminating a hard
glottal attack is to help the child produce relaxed speech with decreased
airflow and subglottic air pressure. It may prove beneficial to compare the
child’s voice to his/her peer’s to help him/her distinguish the difference.
Other techniques such as the whisper-phonation technique, yawn-sigh, chant,
chewing, and usage of Visi-Pitch, can be implemented to eliminate the hard
glottal attack.
Open Mouth: The goal of this facilitative technique is for the
child with vocal hyperfunction to practice having a more open mouth while
phonating and listening. This relaxes the vocal mechanism, thus necessitating
less energy to produce easy speech. The SLP can use a mirror and a puppet to
help this method.
Masking: Otherwise known as the Lombard test, this technique
involves masking the child’s voice by preventing him/her from hearing it while
s/he reads a passage, then playing it back for the child to “find his voice” and
hear the change in phonation.
Pushing: Pushing is a technique in which the child physically
pushes his arms downward during phonation. As the child’s conversational speech
increases in loudness, this technique is slowly diminished.
Yawn-Sigh: The SLP teaches the child about the effects of a yawn
to increase inspiration. Then the SLP explains to the child that that his/her
best voice is produced when the vocal folds are relaxed which is at the end of
the yawn. This technique begins with a sign, vowels, and then single words, and
gradually fades away. According to Boone (2005), this technique is “one of the
most effective therapy techniques for minimizing the tension effects of vocal
hyperfunction.”
There are numerous techniques and methods that a speech and language pathologist can
employ to treat hyperfunctional voice disorders in children. These methods aim
to decrease detrimental vocal behaviors, change the format of voice production,
and enable the healing of vocal fold tissue due to injury. Research has proven
voice therapy to be effective, either alone or in conjunction to other treatment
methods such as surgery or medications (Branski, 2011).
Intervention for vocal hyperfunction in children consists of education, which includes
awareness of voice behaviors and altering improper vocal behaviors, vocal
hygiene programs, direct vocal therapy, and generalization activities. Surgery
is an option, yet is often not preferred ("Hyperfunction Kids," n.d.).
Factors to consider:
An SLP must weigh various factors before procuring a treatment plan. The individual
child and his/her disorder must be assessed holistically. Therapy decisions
depend largely on the age of the child. Boone (2005) states that vocal
hyperfunction, a functional disorder likely caused by vocal polyps or nodules,
is the most common voice disorder found in children. He cautions the therapist
to clarify the cause of the voice disorder prior to planning intervention, as if
an organic or neurological etiology is present, a different treatment plan may
be necessary.
There are other factors to consider to assist an SLP determine an
appropriate intervention plan. These include: “vocal fold tissue health, vocal demands
of the patient, baseline phonatory behaviors, and patient compliance.” The
therapist must bear in mind that different clients with identical disorders may
require different therapies (Branski, 2011).
Goals of therapy:
All hyperfunctional voice disorders are characterized by increased laryngeal and/or
supralaryngeal muscle tension. The primary goal of treatment is to decrease this
tension during voice production, thereby improving one’s voice (Branski, 2011). Additionally,
the goal of therapy is to ingrain in the child a “healthy, non-abusive voice
production pattern (Latrobe, n.d.)." By reducing laryngeal hyperfunction and increasing
laryngeal health, the possibilities of edema, vocal nodules, polyps, and contact
ulcers will be decreased, thereby improving one’s voice and removing the
necessity of surgery("Hyperfunction Kids," n.d.).
Facilitating Techniques:
There are many facilitating techniques that can be employed to help improve the voice
of children with vocal hyperfunction. Boone et al. (2005) suggests the following
techniques: changing horizontal/vertical focus, changing loudness, chewing,
establishing a new pitch, eliminating hard glottal attack, opening mouth,
counseling, masking, pushing, and the yawn-sigh technique.
Prior to implementing facilitative techniques, it is crucial for the SLP to assist the
child in identifying the misuse and abuse of his/her speech mechanism. A
baseline of misuse should be established. If the child is aware of the instances
in which s/he misuses his/her voice, s/he may automatically decrease such
instances. Tally marks or other graphs can be used, to visually show the child
of his/her progress ("Hyperfunction Kids," n.d.). Additionally, the SLP would counsel the child and help
him/her identify the problem and its implications.
Changing horizontal/vertical focus: Sometimes a child produces
sounds by holding the tongue too far back or high in the oral cavity, yielding a
deep voice, or holding the tongue too high or to the front, yielding a thin,
babyish voice. The SLP could utilize imagery to help the client change the focus
of where the voice is being made.
Changing loudness: This method is employed if one’s voice is
excessively loud or soft. A hearing test should be administered to rule out
other possibilities for an overly loud voice. Dr. Boone suggests a five step
process to lessen the loudness including a whisper, quiet voice, normal voice,
talking across the room voice, and yelling. To increase one’s loudness,
techniques such as discussing the reason of the quiet voice, letting the child
listen to a recording of his/her voice, establishing an appropriate pitch level,
and respiration training, can be employed.
Chewing: The purpose of this technique is to teach the child to
open his/her mouth while speaking, to decrease the tension or strain. The child
should look in a mirror while opening and closing mouth in an exaggerated
chewing motion. Then the child slowly says one-syllable words, and then longer
words, and then phrases, while still chewing. The chewing is decreased after a
duration of therapy.
Establishing a new pitch: The purpose of establishing a new pitch
is to “improve vocal quality and loudness (Boone et al., 2005).” The SLP plays a
recording of the child’s voice, then imitates a pitch, as well as uses a pitch
analyzer (i.e. Visi-Pitch.) Once an appropriate pitch is found, the child can
begin to practice speaking with it.
Eliminating Hard Glottal Attack: The purpose of eliminating a hard
glottal attack is to help the child produce relaxed speech with decreased
airflow and subglottic air pressure. It may prove beneficial to compare the
child’s voice to his/her peer’s to help him/her distinguish the difference.
Other techniques such as the whisper-phonation technique, yawn-sigh, chant,
chewing, and usage of Visi-Pitch, can be implemented to eliminate the hard
glottal attack.
Open Mouth: The goal of this facilitative technique is for the
child with vocal hyperfunction to practice having a more open mouth while
phonating and listening. This relaxes the vocal mechanism, thus necessitating
less energy to produce easy speech. The SLP can use a mirror and a puppet to
help this method.
Masking: Otherwise known as the Lombard test, this technique
involves masking the child’s voice by preventing him/her from hearing it while
s/he reads a passage, then playing it back for the child to “find his voice” and
hear the change in phonation.
Pushing: Pushing is a technique in which the child physically
pushes his arms downward during phonation. As the child’s conversational speech
increases in loudness, this technique is slowly diminished.
Yawn-Sigh: The SLP teaches the child about the effects of a yawn
to increase inspiration. Then the SLP explains to the child that that his/her
best voice is produced when the vocal folds are relaxed which is at the end of
the yawn. This technique begins with a sign, vowels, and then single words, and
gradually fades away. According to Boone (2005), this technique is “one of the
most effective therapy techniques for minimizing the tension effects of vocal
hyperfunction.”
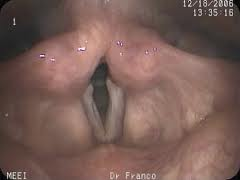
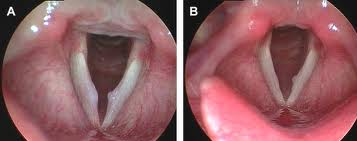
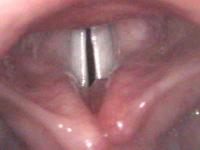
Left vocal polyp with reactive callus
Vocal Hyperfunction
This video, from Mayo Clinic, shows Vocal Cord Therapy. Although it may be more relevant to adult vocal hyperfunction, many of its aspects can be applied to therapy in children with vocal hyperfunction.
Muscle Tension Dysphonia:
Muscle tension dysphonia is also considered a functional dysphonia. Facilitative
techniques that may prove beneficial include “vocal hygiene, care of the voice,
relaxation techniques and counseling.” Additionally, humming exercises, voice
projection, postural positioning, and relaxation exercises may be employed.
Often, medication is necessary to reduce tension of the larynx and adjacent
muscles, as voice therapy alone is not sufficient. These medications may help
improve symptoms related to vocal hyperfunction including laryngoesophageal
reflux, steroid inhaler therapy, or a chronic postnasal drip which may cause
chronic pharyngolaryngitis (Boone, et al., 2005).
Medication:
There are various research studies in which medications were assessed to determine
their efficacy in improving vocal hyperfunction. These studies were done on
adults, yet the results can possibly be transferred to children as well.
Midazolam is a sedative pill, which was given to dysphonic patients in a small
dosage to help them relax their mechanism. This method was proven effective.
According to Bhalla et al (2005), there is not sufficient evidence that Botox is
effective for muscle tension dysphonia although it is used for other voice
impairments.
Other Treatment Methods/Aspects:
Family Support
Aside from actual therapy, indirect therapy, including support from family, is
necessary. It may be pertinent to change the culture of the home. Many
activities and behaviors in the home may need to be controlled to decrease
misuse of the vocal folds. Educating the child, parents, teachers, and family
about the harms caused by vocal misuse is a critical factor in indirect therapy.
The child’s parents should help change the child’s vocal behaviors, in addition
to changing their reaction to the child’s behaviors. This will help the child
carry over and generalize the techniques learnt in therapy ("Hyperfunction Kids," n.d.).
Group Therapy:
Another therapeutic venue that may prove beneficial is group therapy. The therapist in
charge of the session would gather acoustic measures from each child with an
instrument such as the Visi Pitch, analog, or digital voice recorder. The
children in the group could then discuss various techniques that may improve
their voices. By listening to peers’ voices with similar disorders, a child may
better understand the impairment and learn how to facilitate proper
vocalization ("Hyperfunction Kids," n.d.). Additionally, the children may gain support and motivation
from working with peers their age.
Education:
Education is a crucial aspect of the treatment procedure. The SLP should educate the
child, family, and teachers about the causes, nature, risk factors, and symptoms
of vocal hyperfunction. It is helpful to demonstrate to the child the normal
anatomy of the voice box and what occurs due to hyperfunction. Visual aids are a
successful method of teaching. The school teacher could be asked to implement
educational programs during school sessions including “taking care of your
voice,” or “the respiratory system.” Appropriate speech behaviors including
turn-taking, appropriate loudness, not shouting to people in a far distance, and
avoiding interrupting, should be taught as well.
Additionally, a reward and reminder system can be implemented. This
will reinforce proper vocal behaviors as well as develop motivation and
self-esteem. Some ideas include:
Rewards
**Rewards such as stickers, games, or candy can be given to the
child.
**Charts to record the child’s homework, use of vocal strategies, or
water consumption can be created.
**The clinician can provide and decorate a special water bottle with the
child to encourage adequate hydration.
Reminders
**Place notes around the classroom and/or
home.
**Make a computer screen-saver
reminder.
**Charts could be placed on obvious places such as the refrigerator to
remind the child
Psychosocial:
There are many psychological factors that may be present when one is
diagnosed with a voice disorder and must receive treatment. The SLP and/or
parents may find it necessary to provide the child with counseling and
encouragement. The activities implemented in therapy should be designed to boost
the vocal confidence and self-esteem of the child (Latrobe, n.d.).
Research:
In her article, Treatment of Voice Disorders in Children,Hooper (2004),
addressed the necessity to provide data showing prevalence and incidence of
successful treatment of voice disorders in children, primarily vocal
hyperfunction. She states that, while it is known that treatment does work,
sufficient researched data is not properly available. Therefore, the goal of
this article is to provide answers to basic questions on this topic, by
presenting a summary of previous published literature. Questions discussed
include “what are voice disorders?” “who are the children with voice
disorders,” “do children need voice treatment?” among others. This article is a
valuable source for those pursuing treatment of children with vocal
hyperfunction (Hooper 2004).
Muscle tension dysphonia is also considered a functional dysphonia. Facilitative
techniques that may prove beneficial include “vocal hygiene, care of the voice,
relaxation techniques and counseling.” Additionally, humming exercises, voice
projection, postural positioning, and relaxation exercises may be employed.
Often, medication is necessary to reduce tension of the larynx and adjacent
muscles, as voice therapy alone is not sufficient. These medications may help
improve symptoms related to vocal hyperfunction including laryngoesophageal
reflux, steroid inhaler therapy, or a chronic postnasal drip which may cause
chronic pharyngolaryngitis (Boone, et al., 2005).
Medication:
There are various research studies in which medications were assessed to determine
their efficacy in improving vocal hyperfunction. These studies were done on
adults, yet the results can possibly be transferred to children as well.
Midazolam is a sedative pill, which was given to dysphonic patients in a small
dosage to help them relax their mechanism. This method was proven effective.
According to Bhalla et al (2005), there is not sufficient evidence that Botox is
effective for muscle tension dysphonia although it is used for other voice
impairments.
Other Treatment Methods/Aspects:
Family Support
Aside from actual therapy, indirect therapy, including support from family, is
necessary. It may be pertinent to change the culture of the home. Many
activities and behaviors in the home may need to be controlled to decrease
misuse of the vocal folds. Educating the child, parents, teachers, and family
about the harms caused by vocal misuse is a critical factor in indirect therapy.
The child’s parents should help change the child’s vocal behaviors, in addition
to changing their reaction to the child’s behaviors. This will help the child
carry over and generalize the techniques learnt in therapy ("Hyperfunction Kids," n.d.).
Group Therapy:
Another therapeutic venue that may prove beneficial is group therapy. The therapist in
charge of the session would gather acoustic measures from each child with an
instrument such as the Visi Pitch, analog, or digital voice recorder. The
children in the group could then discuss various techniques that may improve
their voices. By listening to peers’ voices with similar disorders, a child may
better understand the impairment and learn how to facilitate proper
vocalization ("Hyperfunction Kids," n.d.). Additionally, the children may gain support and motivation
from working with peers their age.
Education:
Education is a crucial aspect of the treatment procedure. The SLP should educate the
child, family, and teachers about the causes, nature, risk factors, and symptoms
of vocal hyperfunction. It is helpful to demonstrate to the child the normal
anatomy of the voice box and what occurs due to hyperfunction. Visual aids are a
successful method of teaching. The school teacher could be asked to implement
educational programs during school sessions including “taking care of your
voice,” or “the respiratory system.” Appropriate speech behaviors including
turn-taking, appropriate loudness, not shouting to people in a far distance, and
avoiding interrupting, should be taught as well.
Additionally, a reward and reminder system can be implemented. This
will reinforce proper vocal behaviors as well as develop motivation and
self-esteem. Some ideas include:
Rewards
**Rewards such as stickers, games, or candy can be given to the
child.
**Charts to record the child’s homework, use of vocal strategies, or
water consumption can be created.
**The clinician can provide and decorate a special water bottle with the
child to encourage adequate hydration.
Reminders
**Place notes around the classroom and/or
home.
**Make a computer screen-saver
reminder.
**Charts could be placed on obvious places such as the refrigerator to
remind the child
Psychosocial:
There are many psychological factors that may be present when one is
diagnosed with a voice disorder and must receive treatment. The SLP and/or
parents may find it necessary to provide the child with counseling and
encouragement. The activities implemented in therapy should be designed to boost
the vocal confidence and self-esteem of the child (Latrobe, n.d.).
Research:
In her article, Treatment of Voice Disorders in Children,Hooper (2004),
addressed the necessity to provide data showing prevalence and incidence of
successful treatment of voice disorders in children, primarily vocal
hyperfunction. She states that, while it is known that treatment does work,
sufficient researched data is not properly available. Therefore, the goal of
this article is to provide answers to basic questions on this topic, by
presenting a summary of previous published literature. Questions discussed
include “what are voice disorders?” “who are the children with voice
disorders,” “do children need voice treatment?” among others. This article is a
valuable source for those pursuing treatment of children with vocal
hyperfunction (Hooper 2004).